The Pace of Prescribing: What Drives Clinicians to Adopt New Treatments
Physicians are evaluating new therapies – Sermo data reveals what guides their decisions

The healthcare landscape is always evolving, bringing clinicians a steady stream of newly approved therapies and indications. Each one presents the possibility of improved patient outcomes, but also prompts important questions: What does the evidence show? How does this compare to current options? And when is the right moment to begin prescribing?
To understand how physicians navigate this evolving reality, Sermo surveyed 228 U.S. physicians across specialties* to assess how they evaluate new treatments, how quickly they integrate them into practice, and what information they rely on most. The findings illuminate a clinician community that is both deeply committed to innovation and exceptionally thoughtful in how they adopt it.
This data offers a roadmap for life science leaders seeking to support physicians more effectively: what to communicate, when to communicate, and how to enable confident, informed decision-making at every stage of the launch journey.
Clinicians Are Actively Engaging with New Treatment Options
Across the care landscape, physicians are steadily incorporating emerging therapies into practice. Their approach is thoughtful and consistent, reflecting a commitment to staying current, evaluating new evidence, and ensuring patients have access to the most relevant treatment options available.

In the last three months, 70% of clinicians have introduced a newly launched pharmaceutical brand into their practice, and 73% have prescribed a newly approved indication for an existing therapy. These figures illustrate a medical community that is not only aware of innovation but regularly integrating it into everyday clinical decisions.
Clear evidence is central to this readiness. A large majority, 82%, report that they adopt newly approved indications quickly once the supporting data is compelling. Strong trial results and transparent safety information help clinicians feel confident in bringing new options to their patients.
Another important theme is the active pursuit of information. 81% of physicians look for opportunities to use innovative therapies soon after they become available, and 80% seek out details about new treatment options as part of their ongoing learning. Many clinicians are not waiting for updates to reach them. Instead, they are scanning for developments that may enhance care.

Taken together, these patterns reflect a clinical community that is engaged, evidence focused, and continually assessing how new advancements can strengthen treatment strategies.
Peers Are the Most Trusted Source of Early Treatment Insights
Even with the evolution of digital medical education and scientific communication, one factor remains constant: clinicians trust their peers.

This reliance on peer experience underscores a fundamental truth: while clinical data provides the foundation, peer insight provides confidence. Real-world use cases, early success stories, practical workflow advice, and candid reflections on patient tolerability give clinicians the contextual grounding they need to make informed decisions.
This is precisely why peer-led forums, whether in-person, virtual, or community-based, play such an important role in shaping early adoption patterns.
Data Builds Confidence—Especially Early Real-World Evidence
While peer insights offer practical grounding, data remains the linchpin of clinical decision-making.
An overwhelming 84% of physicians say access to early clinical and real-world data increases their confidence in considering a new brand for future prescribing.
This finding reinforces what has long been observed in successful launches: early clarity matters. Clinicians need transparent, digestible evidence that helps them evaluate whether a therapy will meaningfully improve patient outcomes. That includes trial results, safety signals, comparative performance, and real-world outcomes that validate clinical promise in everyday practice.
Early real-world evidence, even in limited form, is especially powerful because it bridges the gap between highly controlled trial environments and the variability of real-world patient populations. It helps clinicians anticipate what they will see in their own clinics, with their own patients.
What Physicians Need Before and After Approval
Physicians’ information needs evolve significantly as a therapy transitions from pre-approval evaluation to post-approval implementation.
Before approval, clinicians concentrate on understanding the therapy’s scientific foundation. They want clarity on how trials were designed, which patient populations were included, and whether the efficacy and safety signals are strong and credible. Comparative context and early real-world insights also help them assess whether a therapy may fill a meaningful gap in current care.
After approval, the focus shifts to practicality. Clinicians look for concise summaries that distill the core evidence, clear comparisons against the standard of care, and deeper understanding of the safety profile as they prepare to discuss the therapy with patients. Real-world performance becomes even more influential, and mechanism of action information helps them explain treatment rationale to both staff and patients as they integrate the therapy into practice.
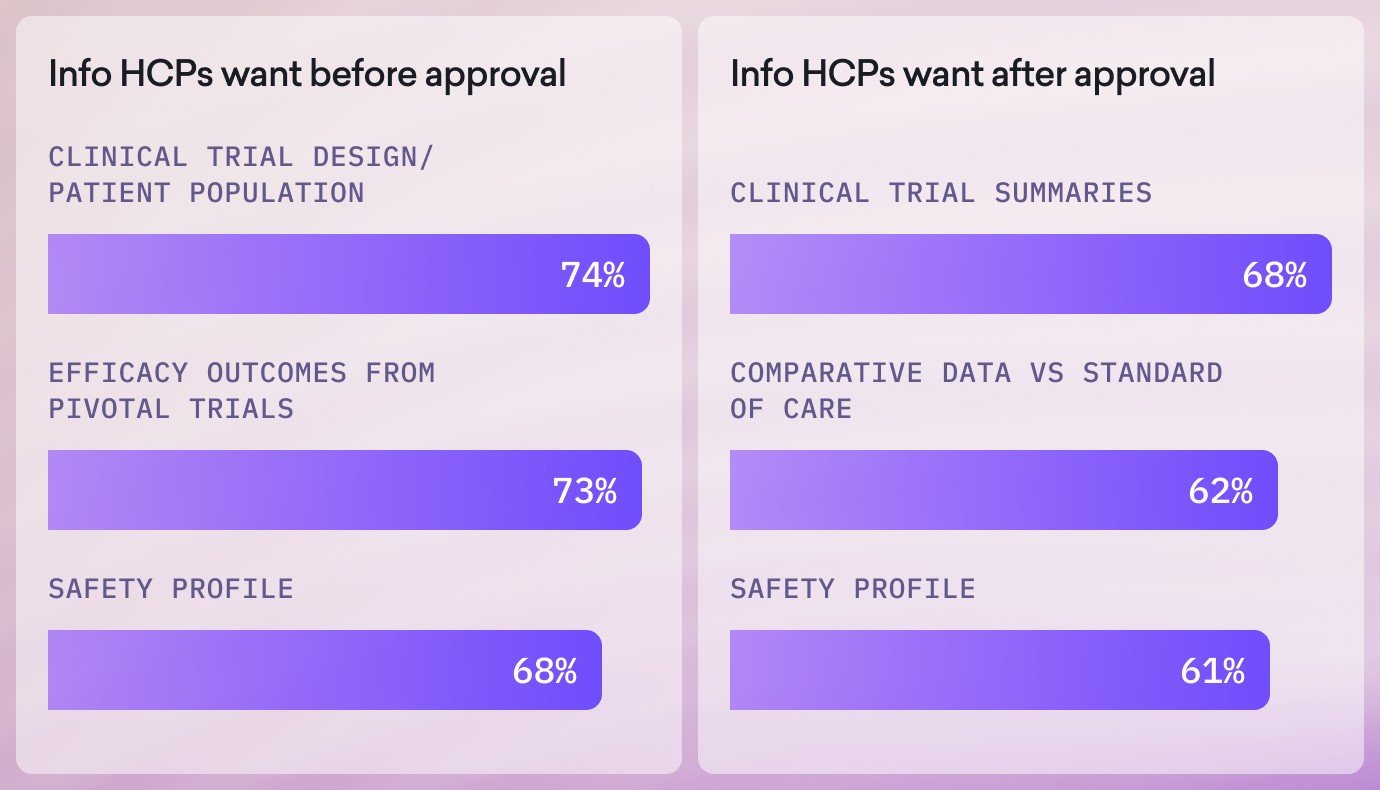
Together, these two phases reflect the dual decision-making process clinicians navigate: first assessing scientific validity and then evaluating clinical usability. Launch strategies that address both needs enable faster, more confident adoption.
What Drives and Delays Earlier Prescribing
Sermo also asked physicians which types of information or resources from pharmaceutical companies would encourage them to prescribe a new brand or indication earlier. Their responses reveal a clear pattern: clinicians do not want more information. They want information that is clearer, more practical, and easier to apply in real-world care.
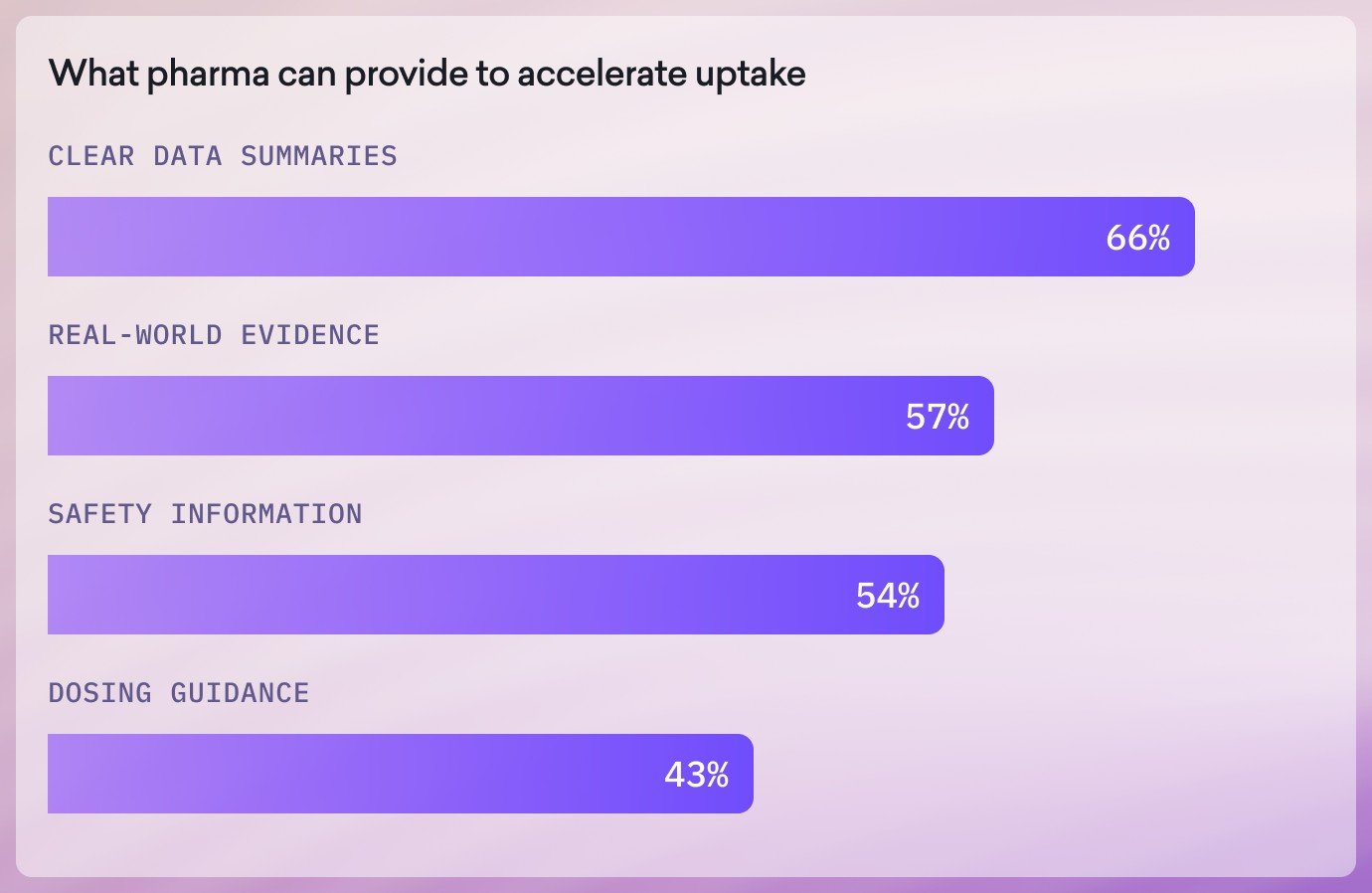
At the same time, the research highlights what slows adoption. Safety concerns remain the biggest barrier (34%), followed by unclear differentiation from existing treatments (18%), lack of practical guidance (13%), and reimbursement uncertainty (11%).
These findings highlight an important dynamic in physician decision-making. Clear, practical information can accelerate adoption, while uncertainty around safety, differentiation, or real-world use can slow it down.
How Content Format Influences Early Adoption
Just as important as what information physicians receive is how that information is delivered. Clinicians respond best to formats that make complex information easy to absorb quickly. Visual summaries, peer discussions, and concise digital formats all help physicians interpret new data more efficiently and translate it into clinical decision-making.
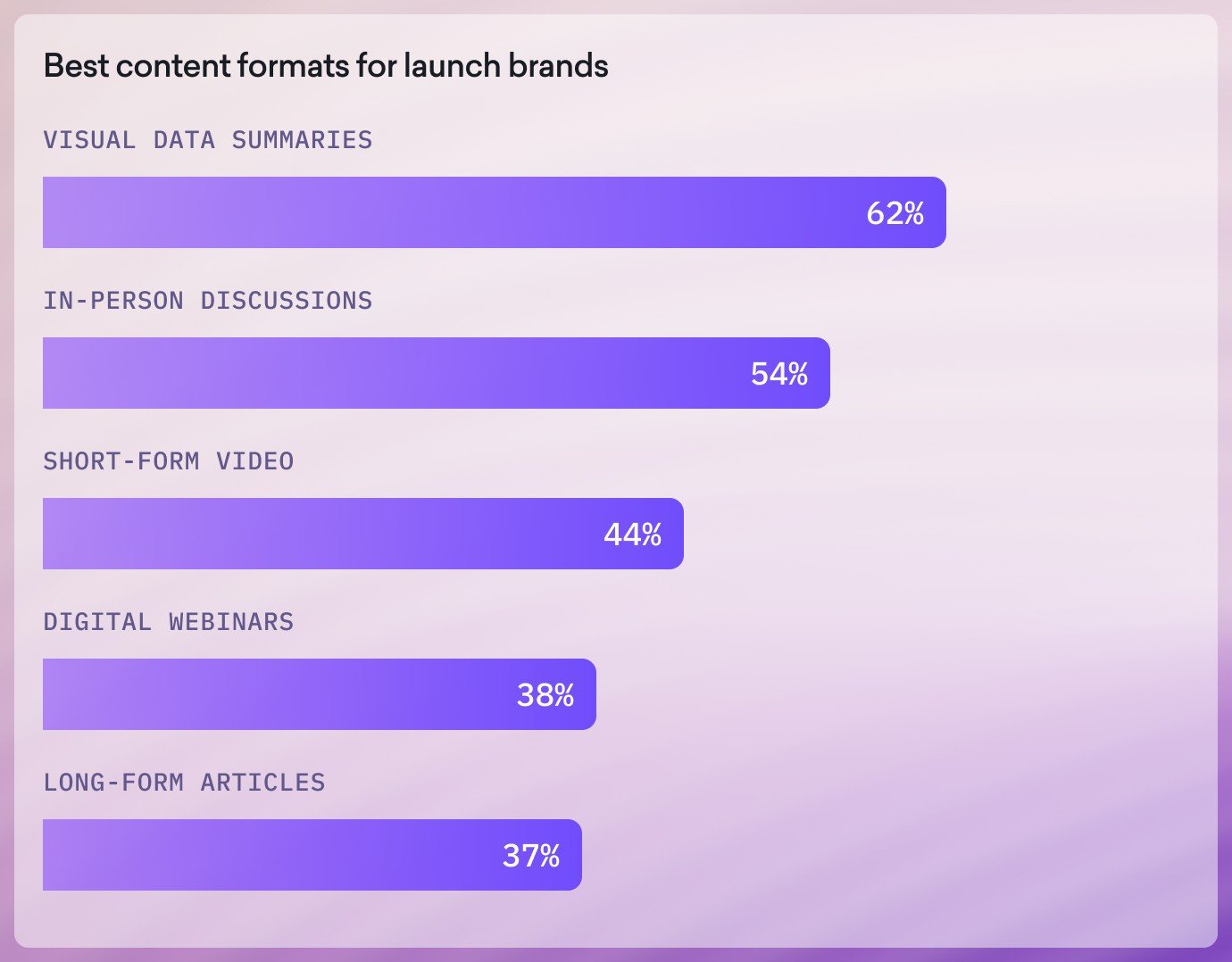
For pharmaceutical companies launching new therapies, this underscores the importance of presenting evidence in ways that are clear, skimmable, and easy to share, helping physicians understand not just the science behind a therapy, but how it fits into real-world patient care.
A Clinician Community Ready for What’s Next
Research findings point to a clinical community that stays closely connected to emerging science while grounding decisions in real-world experience. Physicians follow new therapies with intention, evaluate evidence with care, and rely on peer insight to understand how treatments perform in practice. This combination of curiosity, critical thinking, and collaboration shapes how new options move from approval to everyday care.
Across adoption and information-seeking patterns, a clear theme appears. Strong data accelerates awareness, while shared clinical experience provides the context that helps physicians decide how and when to use a new therapy. Both elements work in parallel, creating a balanced approach that supports thoughtful, confident prescribing.
Sermo will continue to surface these perspectives, so clinicians and life science partners can better understand how treatment decisions evolve in an ever-changing landscape.
Explore how Sermo can support your launch brand with HCP insights and engagement solutions. Request a demo here!
*Specialties include cardiology, dermatology, endocrinology, gastroenterology, neurology, oncology, ophthalmology, pulmology




























